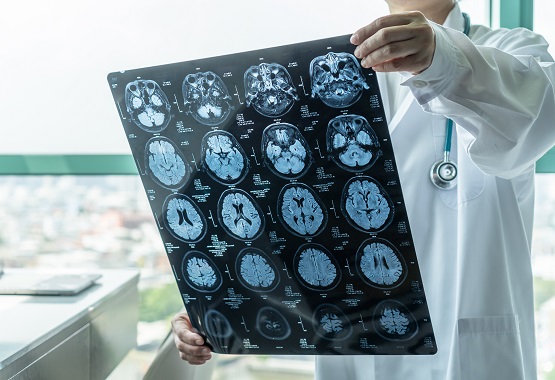
Transient ischemic attacks (TIAs) are sudden and brief neurological events that leave no permanent damage but can warn of an impending stroke. Dr Queck Kian Kheng, Consultant Neurologist, KK Queck Neurology Centre, explains how they occur, who is at risk, and how they can be prevented.
SYMPTOMS AND SIGNS
TIAs have a range of symptoms including numbness, weakness in one part of the body, and speech and visual disturbance. Patients may describe an inability to talk or speak fluently, or an inability to understand he conversation. Visual symptoms include sudden loss of vision in one side of the eye, or loss of vision in a certain part of the vision field.
An easy way to remember the signs of a TIA or stroke is the acronym ‘F.A.S.T.’, which stands for:
Face drooping
Arm weakness
Speech difficulty
Time to call 995!
“A TIA should always be treated as a medical emergency,” emphasised Dr Queck. “Early diagnosis and treatment can prevent a more serious and potentially debilitating stroke.”
CAUSES AND RISK FACTORS
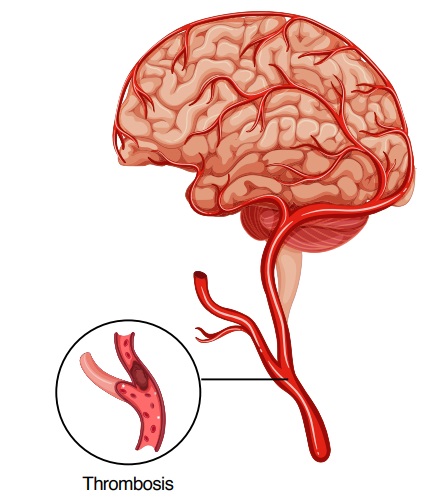
Causes that could lead to a TIA include blockage of the vessels within the brain, known as thrombosis; floating blood clots blocking the vessel within the brain, known as an embolism; and reduced blood flow to the brain due to the narrowing of the blood vessels supplying the brain tissues, called hypoperfusion.
Patients who have underlying risk factors including diabetes mellitus (high sugar level), hypertension (high blood pressure) and hyperlipidaemia (high cholesterol) are at risk of having a TIA. Smoking, a sedentary lifestyle and obesity also heighten the risk factor for TIA.
In younger patients, a significant family history of TIA and/or stroke, and an underlying history of thicker blood, known as the pro-thrombotic state, also increase the risk for TIA.
DIAGNOSIS AND LOOKALIKE CONDITIONS
A TIA is diagnosed on the basis of a patient’s clinical symptoms and presentation. Evaluation with brain scans, either a CT or MRI brain scan, is usually performed to exclude the presence of any underlying bleeding in the brain.
In cases where the TIA is a ‘warning stroke’, and the neurological symptoms are transient, the brain imaging will be normal and show no radiological evidence of acute stroke.
A thorough clinical diagnosis is critical, since there are many other neurological conditions that can mimic the symptoms of a TIA, according to Dr Queck. These include migraine disorder, nerve lesion, and electrolyte disorders like hypoglycaemia (low blood sugar level).
TREATMENT AND MANAGEMENT
When a patient suffers a TIA, the priority is to identify the cause, and treat the symptoms accordingly. The second priority is to prevent the future occurrence of a stroke.
Once the cause of the TIA has been established, blood thinning medication will typically be prescribed to reduce the risk of another TIA or a stroke occurring in the future. Next, a long-term health plan with actionable goals should be developed, implemented and monitored. The aim is to control the patient’s underlying risk factors such as diabetes mellitus, hypertension and hyperlipidaemia.
If untreated, a TIA may be followed by a serious stoke that leaves the patient with significant functional disability. Early treatment is crucial for secondary stroke prevention.
THE GOOD NEWS
Dr Queck shared, “The good news is that up to 80 percent of TIAs and strokes are preventable with medications and lifestyle modification.” He reiterated the importance of treating a TIA as an emergency, since early treatments have been proven to improve patient outcomes.
“Early discovery helps with recovery,” advised Dr Queck.
In summary, the good news is that with recent advances in medical technologies, TIAs can be treated and prevented. And if you do suffer a TIA, you can take charge of your future health and prevent a stroke by heeding the timely warning.
Article contributed by Dr Queck, an accredited doctor of Mount Alvernia Hospital.
Consultant Neurologist
KK Queck Neurology Centre
Mount Alvernia Hospital Medical Centre A #02-03
Tel: 8891 7996
This article is taken from our My Alvernia Magazine Issue #42/43. Click here to read the issue on our website or on Magzter.