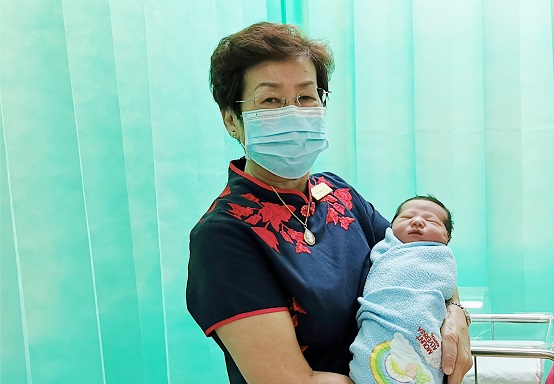
Our veteran midwife, Ng Geok Pin or ‘Sister N.G.’ as she is known amongst her colleagues, Assistant Director of Nursing at Mount Alvernia Hospital, reminisces and reflects on how far midwifery has come during her 45 years of ushering new lives into the world.
THE CONSTANTS AND THE CHANGES
According to N.G., there have been few major changes to the job definition and responsibilities of midwives since 1976, when she first qualified as a midwife and worked at BMI Mount Alvernia Hospital in Guildford, England. The main difference is that back then midwives were allowed to deliver babies in private hospitals without the presence of an obstetrician.
In fact, as N.G. was trained in the UK, she was allowed to not only conduct deliveries but also teach student midwives. In the UK, she even delivered babies at patients’ homes.
Training, too, has remained relatively consistent over the years. In N.G.’s day, only Registered Nurses who had undergone three years of general training could proceed to study for their Advanced Diploma in Midwifery. The same applies today, only an Advanced Diploma in Midwifery now takes eight months to complete compared to the previous 12 months.
MORE EDUCATED PARENTS ARE MORE PREPARED PARENTS
One factor that has had an impact on midwives’ job responsibilities is the mindset of parents. Whereas once fear and confusion reigned, modern parents are generally calmer and more composed, according to N.G., a fact that she attributes to widespread education.
“Thanks to the availability of antenatal classes, today’s new parents are generally well prepared and understand what labour is all about,” said N.G. “They used to be quite fearful and sometimes at a complete loss when the time came to be admitted to the labour ward.”
CHANGES TO ‘NATURAL’ DELIVERIES
Whereas once only the midwife may have been present for a natural delivery following a low-risk pregnancy, today it involves a team of at least three, in addition to mother and child.
“In the old days, there was no placing of the patient’s legs in stirrups. She simply pulled back her thighs and pushed or bore down, following the midwife’s prompts,” recalled N.G. “Today, there are always two nurses and an obstetrician in the delivery room to assist the mother at the point of delivery. One of the nurses may not be a midwife. At times, a paediatrician may also be present if the baby is at risk.”
CHANGES TO ASSISTED AND EMERGENCY DELIVERIES
As for assisted deliveries, little has changed with regard to the instruments used. N.G. shared that Wrigley’s forceps, Neville Barnes forceps and Kielland’s rotational forceps are still used by obstetricians, based on their preference and the position of the baby. The main addition to the ‘toolkit’ is a disposable unit called a Kiwi® cup, which has found favour among obstetricians in recent years.
With regard to caesarean deliveries, N.G. recalled that while parents’ consent used to be obtained by a trained nurse, now the responsibility lies with the obstetrician.
“The obstetrician is now responsible for obtaining consent from the patient. He or she is obliged to explain the nature, indication and possible side effects of the operation,” shared N.G.
THE DELIVERY OF COMFORT
Today, midwives have considerably more resources to draw on for the purposes of comforting a distressed mother.
“Today, we can remind the mother of the breathing exercises that she learnt during her antenatal classes. We can also offer her Entonox gas, a safe form of pain relief that consists of 50 percent oxygen and 50 percent nitrous oxide,” shared N.G. If the patient is fit to get out of bed, music, aromatherapy and warm showers can also help.
What has not changed are the words of encouragement and positive reinforcement that are never far from midwives’ lips. Now that fathers are usually present at their babies’ births, midwives often ask husbands to hold their wives’ hands and do the breathing exercises with them.
N.G. confirmed that sometimes fathers become more emotional than mothers, who are immersed in the physical challenge of giving birth. Midwives comfort anxious fathers in the same way that they always have, with soothing words and a reminder of God’s gift waiting at the end of the ordeal.
“We will patiently explain the progress of the wife’s labour, assuring him that frequent and strong contractions are nature’s way to gradually help the descent of the baby’s head and dilate the mother’s cervix to the 10cm mark, which is when she can bear down and push,” shared N.G. “We will constantly remind him that he will soon see his lovely little bundle of joy!”
PRECIOUS MEMORIES
When we asked N.G. to share some of her fondest memories as a midwife, she provided this litany of meaningful moments.
“Seeing first-time mothers very determined to push their babies out, tearful parents holding their newborn with smiles and tears rolling down at the same time – these are always special moments,” reminisced N.G.
On a more comical though somewhat alarming note, she recalled, “One father fainted as the baby was born. Another fellow got carried away, happily snapping photos of his newborn and overlooking the presence of the wife, who had just endured the hardship of labour. He had completely forgotten all about her until she called out to him and asked him to take a picture of her holding the baby!”
GIVING BIRTH, SHARING HAPPINESS
“Giving birth is a happy occasion. I get the immense job satisfaction of seeing the arrival of newborns and sharing in the happiness of the parents and grandparents,” said N.G.
Midwifery – from all reports, sounds like one of the hardest but happiest jobs in the world.
This article is taken from our My Alvernia Magazine Issue #44. Click here to read the issue on our website or on Magzter.